The festive season is here. It is party time and the food is celebratory and abundant. As a counterpoint, we could consider the levels of nutrition experienced by frail aged people right across the community.
Meals are markers of the day for all of us – but they are especially so for those who have limited mobility or who are confined to the lonely room of an aged-care facility and for those who might be isolated within their suburban home. It is sad then, when the food disappoints and/or has little nutritional value.
We are fortunate in Australia to have the ready availability of fresh, wholesome food. So it is deeply disturbing to learn of the high rate of malnutrition experienced by older Australians. In April this year, the Dietitians' Association of Australia released the results of a study that revealed that 40 percent of older Australians were either malnourished or at risk of malnutrition.
One of the most fulsome exposés of this disgraceful situation was written earlier this year by Joe Lederman from 'Foodlegal lawyers and Consultants' in an article, Elderly at risk: Food deficiencies of Australia's aged population.
This article outlines the many reasons why frail older people are either malnourished or underweight. Lederman suggests that the fixed income of many seniors who remain in their own homes as they age often means that food and grocery expenses are cut as budgets become tight.
In aged-care facilities the lack of sufficient staff to assist with meals is a key factor. Lederman also targets the vague Accreditation Agency's Standard 2.10, that seeks to monitor nutrition as well as the fact that many large facilities contract out the whole preparation of meals to third party contractors who are not directly responsible for the well-being of residents.
A further issue was clearly outlined in a submission by Western Australian Visiting Dentist, Dr. Clive Rogers, to the Productivity Commission Inquiry, Caring for Older Australians. He writes about the diseased mouths he sees in the facilities he visits. Our wish to have our own 'teeth for life' soon becomes 'teeth for infection', 'teeth for pain' or even 'teeth for death' once we enter an aged-care facility as good oral hygiene is rarely maintained. Dr Rogers recognises that caring for another person's oral and dental health is extremely difficult but he, too, is critical of the Accreditation Agency for poor auditing of the Standards and incorrectly acknowledging compliance when it clearly isn't occurring.
Dr Rogers frames his concerns as a human rights issue and notes that there is no formal process for a care-worker who detects medical/dental abuse of a resident to report it.
He makes the point even more starkly with the following:
'If you went to your dentist right now and said, from today:
- I am not going to brush my teeth or gums'
- I am going to stop using a fluoride toothpaste,
- I'm going to eat and drink sugar regularly throughout the day every day.
Your dentist would probably recommend that you have your teeth taken out and dentures put in place because your teeth will very soon become destroyed, and become sources of infection, pain and have a deleterious effect on your general health. This is a fact. This is happening in our RACFs for the last few decades.'
There are many reasons why frail older people are not maintaining adequate levels of nutrition - poor staffing levels and the widespread incident of diseased teeth are just two of them.
But while we are enjoying our festive food this Christmas season, it might be as well to remember those who are malnourished amid all this plenty.
Excerpt from Dr Clive Rogers (Dentist) submission to the Productivity Commission's Caring for Older Australians Inquiry (2010):
Currently we have a large percentage of the population living in Residential Aged Care Facilities who have developed a disability, of one form or another, which prevents them doing even these ADLOH. A significant proportion of these people have been encouraged to keep their natural teeth as 'teeth-for-life'. They are now unable to care for these teeth and I contend that they are becoming 'teeth for infection', 'teeth for pain', and 'teoeth for death'.
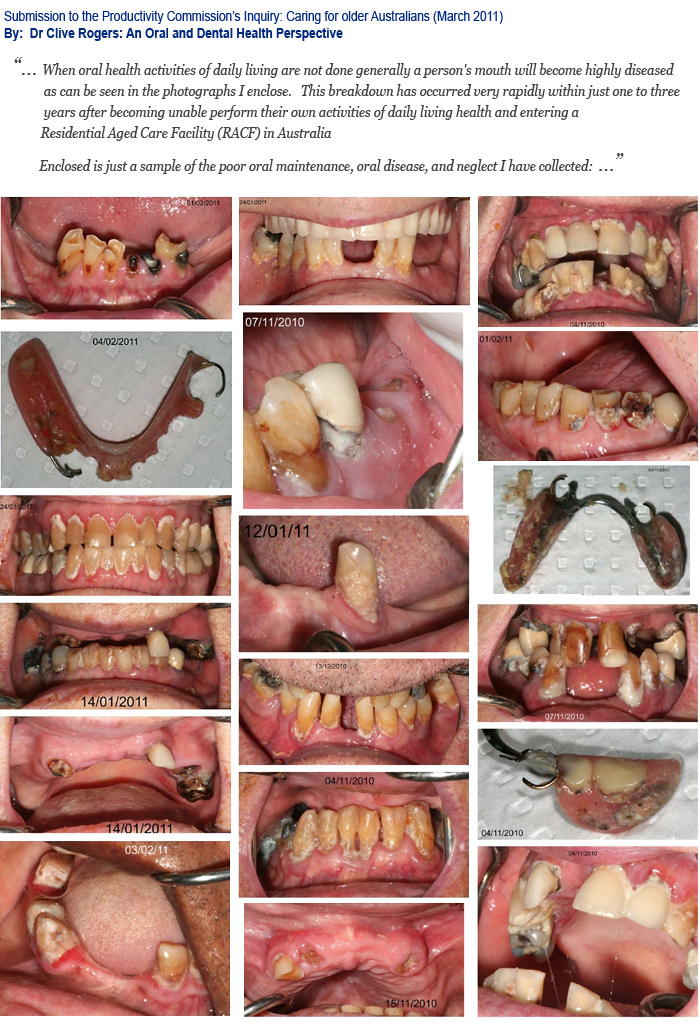
When oral health activities of daily living are not done generally a person's mouth will become highly diseased as can be seen in the photographs I enclose. This breakdown has occurred very rapidly within just one to three years after becoming unable perform their own activities of daily living health and entering a Residential Aged Care Facility (RACF) in Australia.
Enclosed is just a sample of the poor oral maintenance, oral disease, and neglect I have collected. Further examples of this are the Appendix.
It is my overwhelming experience as a dentist who has restricted his practice to special needs, geriatric dentistry, and visiting many patients in RACFs that, a person in RACF with a disability receives inadequate daily oral and dental maintenance care: that is the basic activities of daily living to maintain oral health are not being provided. Even the relatively simple daily activity of cleaning the residents' dentures is generally not being adequately done.
The dentures photographed are covered with stagnate food, which is months old: this is blatant care neglect.